What is Radiation Therapy?
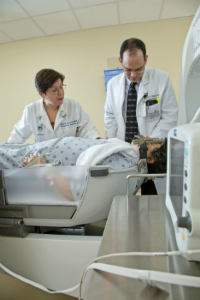
Cancer cells have an increased sensitivity to DNA damage compared to healthy cells, so the goal of radiation therapy, which uses high-energy X-rays, , is to injure or destroy cancer cells by damaging their DNA — making it impossible for the cells to continue to divide and spread.
Although radiation can damage normal cells as well as cancer cells, doses are calculated to minimize exposure to surrounding tissue. If normal cells are impacted, your body will work to repair these normal cells and tissues over time.
To increase the likelihood of a positive outcome, radiation therapy may be paired with other cancer treatments, including:
- Surgery
- Chemotherapy
- Targeted therapy
- Immunotherapy
How is Radiation Therapy Used?
Radiation therapy is typically most effective when used for cancer or tumors that are located in specific parts of the body. Radiation is primarily used to eliminate certain types of cancer, but can be used in other instances, including:
- Neoadjuvant radiotherapy, which is used to shrink tumors prior to surgery. This allows for the tumor to be surgically removed in a less invasive manner.
- Adjuvant radiotherapy, which is intended to destroy microscopic cancer cells remaining in the body after surgery. In some cases, oncologists will treat certain parts of the body where cancer most often spreads in order to reduce the chance of the cancer recurring.
Radiation therapy also can be used as a method of palliative care. For patients whose cancers have spread to other parts of the body, radiation therapy can be used to shrink certain tumors to relieve pain and other symptoms in order to make patients more comfortable.
As medical technology continues to improve, radiation oncologists will have more options available to help deliver highly targeted and even more precise treatments, resulting in less risk to patients and, ultimately, better outcomes.
What to Expect from Radiation Therapy Treatment
If your doctor is recommending radiation therapy to treat your cancer, you may be unsure of what to expect. To better understand how the treatment works and why it may be necessary, we recommend you schedule a consultation with a board-certified radiation oncologist. Afterward, you and your oncologist can discuss your options and develop a treatment plan that’s designed to provide you with the very best chance of success.
Types of Radiation Therapy
Radiation therapy targets the specific parts of the body where tumors or cancer cells are present and differs from other cancer treatments that expose your entire body to intense cancer-fighting medicine. Depending on where your cancer is located, radiation therapy can be delivered through a variety of means, including:
- External beam radiotherapy treatments, a linear particle accelerator (a machine that accelerates electrons or high energy X-rays) is used to deliver beams of high-energy X-rays directly to the site of a tumor.
- Systemic radiation therapy, which involves delivering radioactive substances orally or via an IV, is also designed to focus specifically on the tumor with minimal damage to organs or normal tissue.
- Internal radiation, also known as brachytherapy, involves the implantation of a radioactive source into or near the site of a tumor. Depending on your course of treatment, this implant may be temporary or permanent.
Memorial Hermann provides the following radiotherapy treatment options.
External Beam Radiation Therapy (EBRT)
When you think of “conventional radiation therapy” you’re likely thinking of External Beam Radiation Therapy (EBRT). During EBRT, patients lie down on a treatment table while a linear accelerator (a tool that accelerates electrons or high energy X-rays) delivers a beam, or several beams of radiation to a targeted tumor site. With careful planning, EBRT can destroy cancer cells with minimal damage to surrounding tissue.
Intensity-Modulated Radiation Therapy (IMRT)
Tumors are not perfectly flat or round, which is why it’s important to be as accurate as possible during treatment. Intensity-Modulated Radiation Therapy (IMRT) uses computer-controlled linear accelerators to break up radiation doses into several “beamlets,” which changes the intensity and size of each dose. By reducing the amount of excess radiation exposure to normal tissue, IMRT makes it possible to use higher and more effective radiation doses typically resulting in fewer side effects than conventional radiotherapy techniques.
Image-Guided Radiation Therapy (IGRT)
Image-Guided Radiation Therapy (IGRT) is similar to IMRT, but uses occasional visual scans to provide more precise targeting of the tumor before and during treatment. This addition makes IGRT an effective treatment for cancers in areas of the body where there is excessive motion, such as the lungs and upper abdomen. Before and during treatment, your care provider will take X-rays or CT scans to ensure accurate tumor targeting.
Stereotactic Body Radiotherapy (SBRT)
Originally developed as a highly precise procedure for treating small brain tumors (called stereotactic radiosurgery), SRBT uses similar methods to treat tumors in other parts of the body, and is often utilized to treat early stage lung cancer or to target cancer cells that have spread to other parts of the body.
By combining multiple imaging (X-rays or CT scans), along with localization techniques – including IGRT – and systems to help you stay still during treatment, SBRT can provide radiation delivery that is accurate to within one to two millimeters.
Unlike other types of radiation therapy, SBRT requires very few treatments, ranging from one to five sessions. These sessions can typically be completed in one week or less.
High Dose Radiation Therapy (HDR)
High Dose Radiation Therapy (HDR) is most commonly used for treating gynecologic and prostate cancers. This therapy allows radiation oncologists to administer higher doses of radiation over a shorter period of time, and deliver radioisotopes (the treatment materials) to afflicted areas with minimal damage to surrounding tissue.
Gamma Knife®
The Gamma Knife® procedure does not involve an actual knife – instead, it uses multiple focused radiation beams to target tumors with unparalleled precision. In addition to treating multiple types of brain tumors, this highly specialized, robotic device can also be used noninvasively to treat a number of vascular and functional lesions, including arteriovenous malformations and trigeminal neuralgia.
What Are the Side Effects or Risks of Radiation Therapy?
Like other cancer treatments, patients will react differently to radiation therapy, depending on the type of cancer, the location of the cancer and the amount of and type of radiation prescribed.
Common side effects of radiation therapy can include:
- Fatigue
- Skin irritation
- Hair loss (when treating affected areas)
- Mouth sores (when treating head and neck )
- Problems swallowing (when treating the chest, head or neck)
- Diarrhea (when treating the abdomen, pelvis or stomach)
During or after treatment, you may or may not experience side effects. In general, patients who do their best to maintain a healthy lifestyle before and during treatment are more likely to have a positive experience. The radiation oncologist and your cancer care team understand which side effects may occur, so you can work together to better manage any negative symptoms you may experience.
Why Choose Memorial Hermann for Treatment?
Memorial Hermann Cancer Centers are accredited by the American College of Surgeons’ (ACoS) Commission on Cancer (CoC). This rare distinction is given to cancer programs that uphold the highest standard of care for patients. When you choose Memorial Hermann Cancer Centers for your cancer treatment, you can rest assured you will receive the best possible care delivered by a compassionate team of caregivers in a calm, healing environment.
Contact Us
For more information about Memorial Hermann Cancer Centers, including how to get connected to our support services or an affiliated provider, please call (833) 770-7771 or fill out the form below to be connected to one of our Oncology Nurse Navigators.